Chanarin Dorfman Syndrome
What Is Chanarin Dorfman Syndrome?
Chanarin-Dorfman syndrome (CDS) or Neutral Lipid Storage Disease with Ichthyosis (NLSDI) is an ultra-rare, recessively inherited form of ichthyosis. Males and females are equally affected. It is caused by mutations in the ABHD5 gene (α/β hydrolase domain-containing protein 5) that codes for a protein also known as CGI-58 1,2. This protein is expressed in many tissues of the body and is important in the metabolism of triglyceride lipids. The exact mechanism by which it causes ichthyosis and other abnormalities is not well understood. The clinical description that follows is based on the findings in approximately 50 cases with verified mutations in ABHD5. [REF] Most reported cases have come from the Middle-East or Japan. It is important to note that Neutral Lipid Storage Diseases caused by mutations in genes other than ABHD5 do not have ichthyosis.
Longterm Course
Key Findings
- Skin
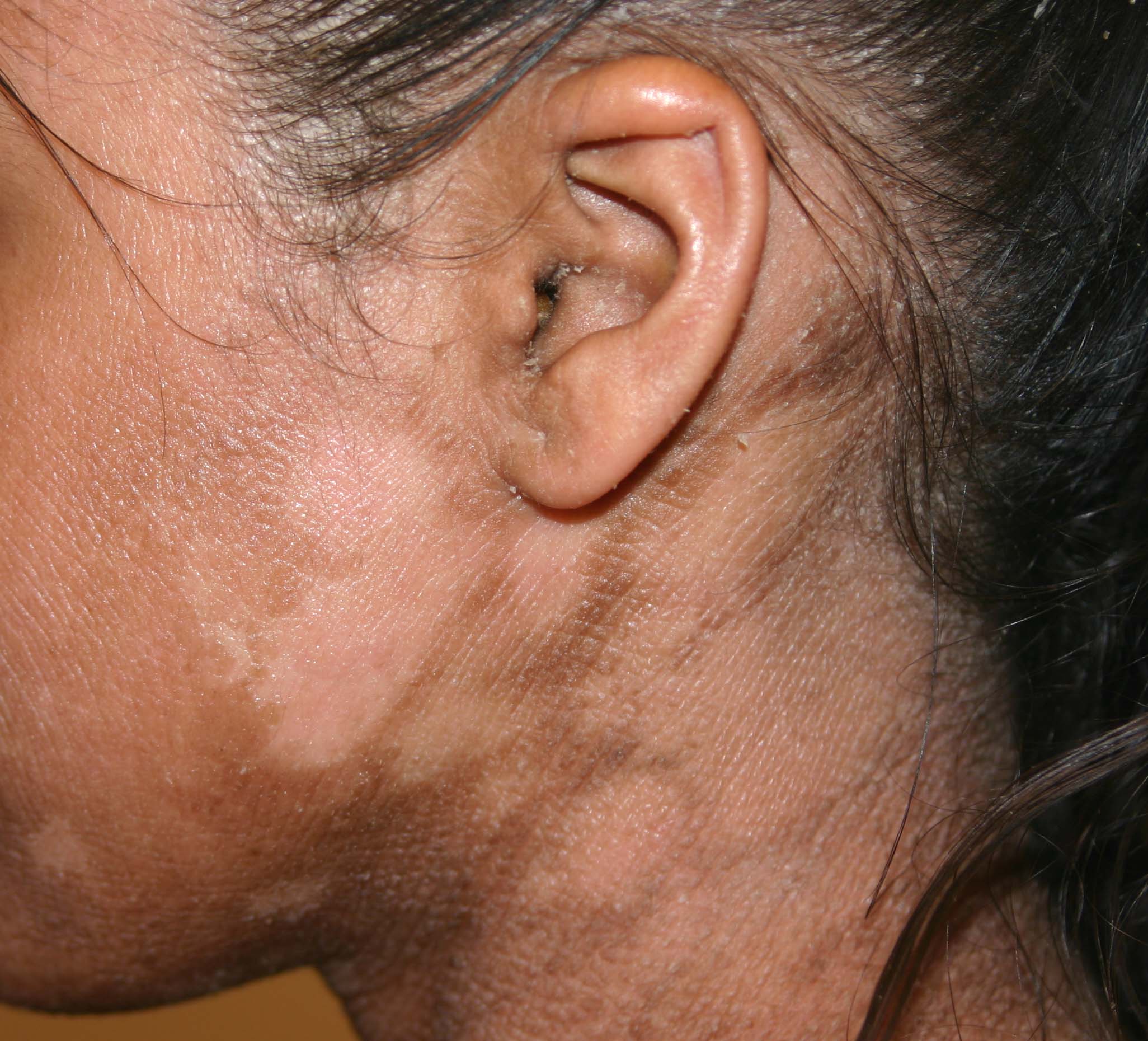
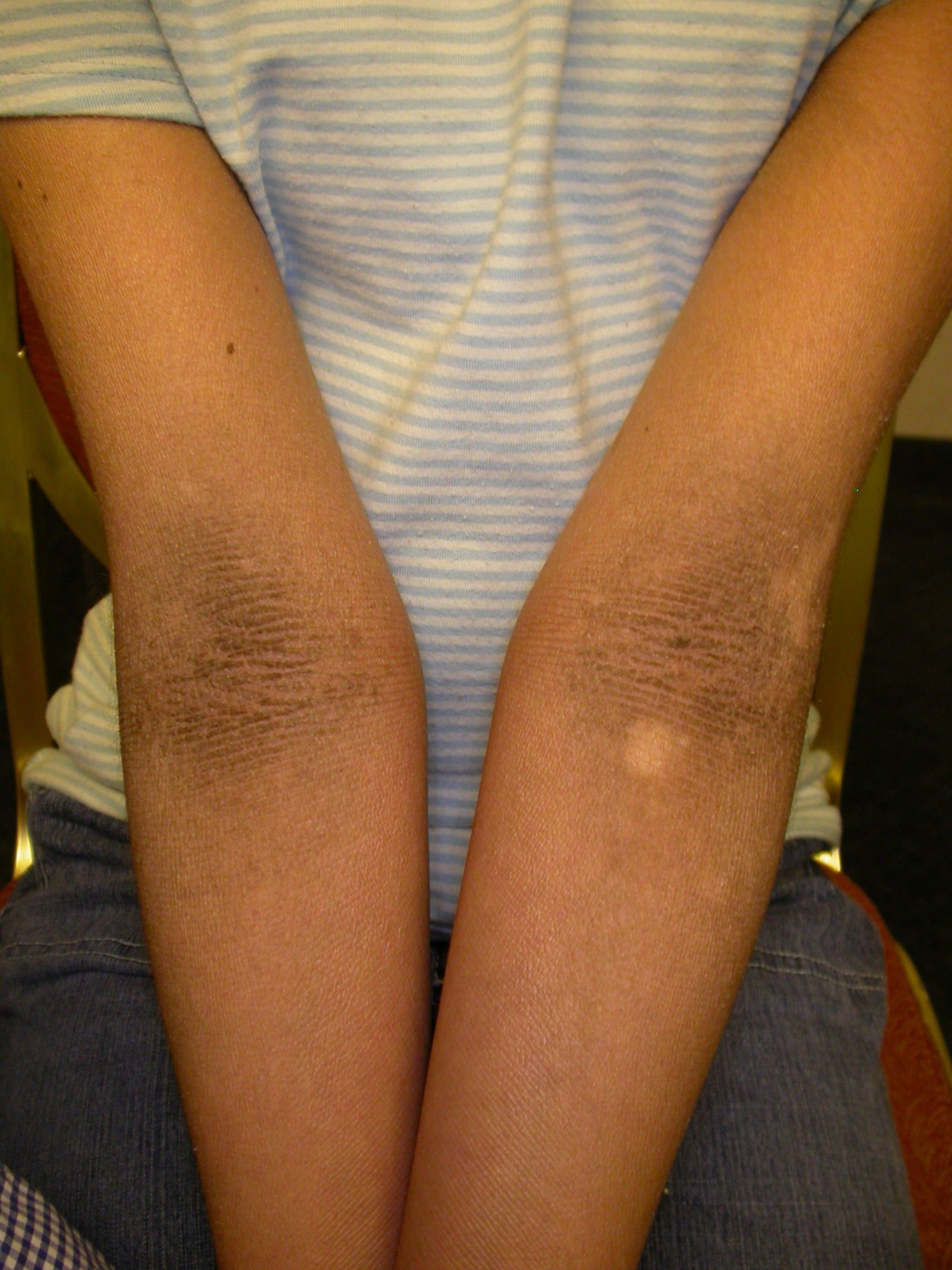
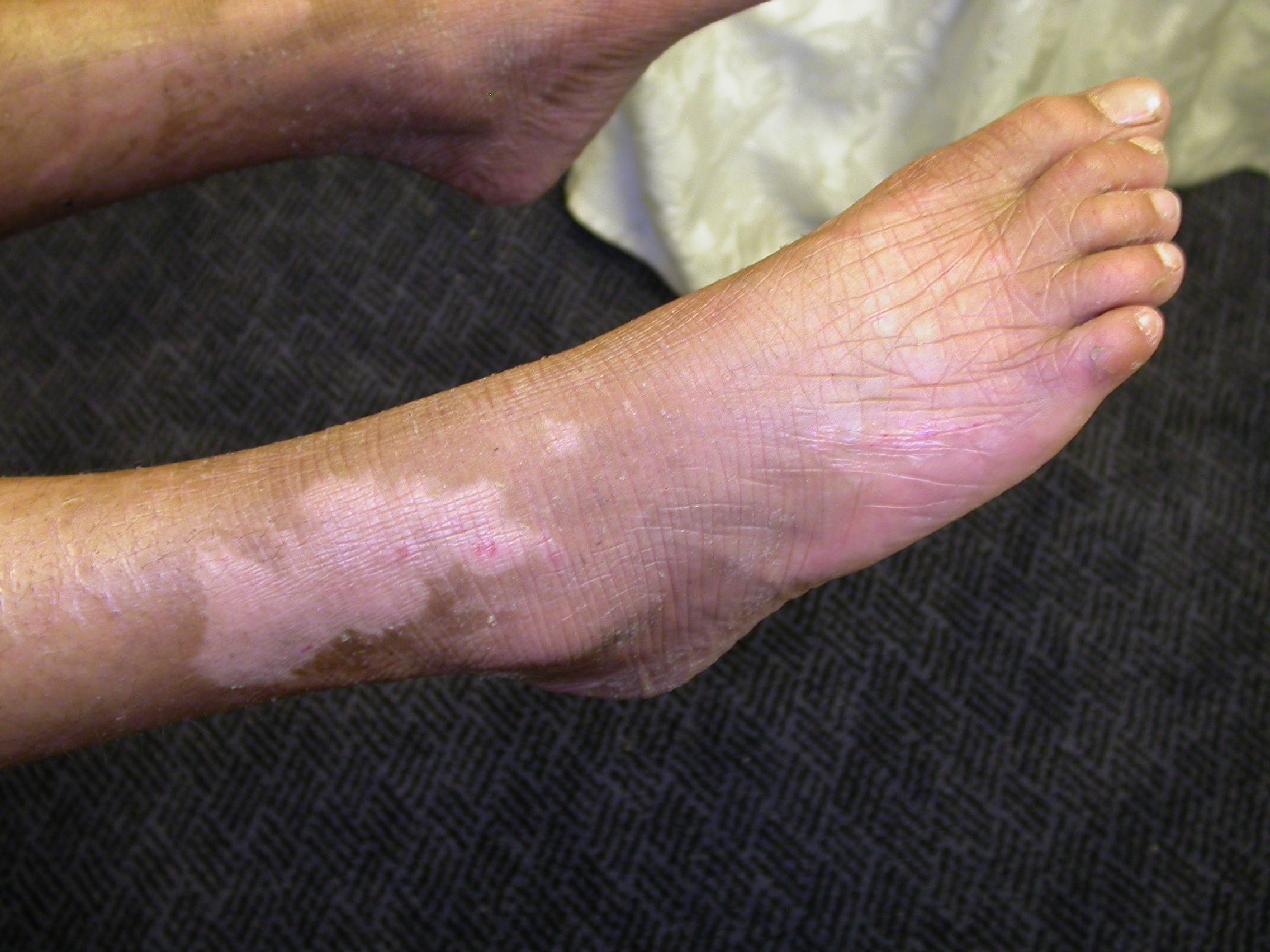
Small, tightly adherent scales and thickening of the epidermis give the appearance of increased skin markings or ridges, especially near body folds; mild erythroderma and eversion of eyelids (ectropion); itching.
Associated Findings
- Eyes
Cataracts and other visual disturbances - Ears
Hearing loss - Neuromuscular
Intelligence usually normal; weakness can be progressive - Liver
Large - Intestine
Malabsorption (rare)
Clinical Resources
- Clinicians seeking to confirm a diagnosis should visit the Edvyce portal to submit a case to experts in ichthyosis.
- Learn more about FIRST’s Resources for individuals and families affected by Ichthyosis?
- Information about current clinical trials and research studies can be found here.
What are the Signs & Symptoms?
All tested individuals have had an enlarged liver, and blood enzymes abnormalities suggest involvement of the liver and muscles. Many are reported to have small or misshaped ears, early cataracts, large spleen, mild deafness and mild muscle abnormalities. In contrast to other forms of NLSD which do not have ichthyosis, the muscle and liver disease in NLSDI is generally less severe and progresses slowly, if at all. Less common findings reported in NLSDI include, strabismus (lazy eye), mental retardation and mild growth retardation. The relationship of these less common findings to the mutation in ABHD5 causing the ichthyosis is not well-established. The effect of mutations in ABHD5 on lifespan is unknown (the oldest reported case so far is 62 y.o.)3. The susceptibility of affected individuals to other common diseases is unknown. Effect on fertility is unknown, although one affected male has had children.
How is it Diagnosed?
Results of genetic tests, even when they identify a specific mutation, can rarely tell you how mild or how severe a condition will be in any particular individual. There may be a general presentation in a family or consistent findings for a particular diagnosis, but it’s important to know that every individual is different. The result of a genetic test may be “negative,” meaning no mutation was identified. This may help the doctor exclude certain diagnoses, although sometimes it can be unsatisfying to the patient. “Inconclusive” results occur occasionally, and this reflects the limitation in our knowledge and techniques for doing the test. But we can be optimistic about understanding more in the future, as science moves quickly and new discoveries are being made all the time. You can participate in research studies and also receive genetic testing through the National Ichthyosis Registry at Yale University or for more information about genetic tests performed you can visit GeneDx, www.genedx.com.
What is the Treatment?
Genetic counseling may be of benefit for affected individuals and their families.
References
- Lefevre C, Jobard F, Caux F, Bouadjar B, Karaduman A, et al. (2001) Mutations in CGI-58, the gene encoding a new protein of the esterase/lipase/thioesterase subfamily, in Chanarin-Dorfman syndrome. American Journal of Human Genetics 69: 1002-1012.
- Redaelli C, Coleman RA, Moro L, Dacou-Voutetakis C, Elsayed SM, et al. (2010) Clinical and genetic characterization of Chanarin-Dorfman syndrome patients: first report of large deletions in the ABHD5 gene. Orphanet J Rare Dis 5: 33.
- Ujihara M, Nakajima K, Yamamoto M, Teraishi M, Uchida Y, et al. (2010) Epidermal triglyceride levels are correlated with severity of ichthyosis in Dorfman-Chanarin syndrome. J Dermatol Sci 57: 102-107.
- Srinivasaraghavan R, Krishnamurthy S, Chandar R, Cassandrini D, Mahadevan S, et al. (2014) Acitretin-responsive ichthyosis in Chanarin-Dorfman syndrome with a novel mutation in the ABHD5/CGI-58 gene. Pediatr Dermatol 31: 612-614.
- Congenital Ichthyosiform Erythroderma (CIE)
- Lamellar Ichthyosis
- Collodion Baby
- Darier Disease
- Epidermal Nevus
- Epidermolytic Ichthyosis
- Erythrokeratodermia Variabilis
- Erythrokeratodermia Cardiomyopathy Syndrome
- Harlequin Ichthyosis
- Ichthyosis Vulgaris
- Ichthyosis with Confetti
- Keratitis-Ichthyosis-Deafness (KID)
- Netherton Syndrome
- Pachyonychia Congenita
- Palmoplantar Keratodermas
- Sjögren-Larsson Syndrome
- X-Linked Ichthyosis
- Chanarin Dorfman Syndrome
- CHILD Syndrome
- Conradi-Hünermann
- Ichthyosis Hystrix with Deafness (HID) Syndrome
- Ichthyosis Hystrix Curth-Macklin
- Refsum Disease
- Trichothiodystrophy
Phenotype Names
Chanarin Dorfman Syndrome, Neutral Lipid Storage Disease, Disorder of Cornification 12 (Neutral Lipid Storage Type), DOC 12 (Neutral Lipid Storage Type), Ichthyosiform Erythroderma with Leukocyte Vacuolation, Ichthyotic Neutral Lipid Storage Disease, Triglyceride Storage Disease Impaired Long-Chain Fatty Acid Oxidation
EDD Name
ABHD5-sEDD
OMIM
Inheritance
Autosomal recessive
Incidence
Very rare
Diagnostic Tests
Lipid inclusions in cells on blood smear or skin biopsy
Age of First Appearance
Birth
Abnormal Genes
PNPLA2 gene, which encodes adipose triglyceride lipase
Primary Symptom Photos