Pachyonychia Congenita
What Is Pachyonychia Congenita (PC)?
Pachyonychia congenita (PC) is a chronically debilitating, ultra-rare genetic skin disorder. PC is caused by a mutation in one of five keratin genes: KRT6A, KRT6B, KRT6C, KRT16, or KRT17. Those with a mutation in KRT6A are named PC-K6a, those with a mutation in KRT6B as PC-K6b and so on. The most striking feature of PC is the painful blistering and callusing on the soles of the feet which severely affects patients’ mobility.
PC follows an autosomal dominant pattern. Autosomal means the genetic defect is carried on one of the 22 human chromosomes that do not determine sex. Dominant means the gene with the mutation dominates over the normal gene. A person with one dominant gene for PC and one gene for normal skin will have PC. Nearly one-half of those with genetically confirmed PC are spontaneous cases, meaning that the disorder is spontaneous and not inherited.
Keratins are proteins that are important to the normal function of hair, nails and skin. Not every affected individual exhibits every clinical feature. Each person with PC may display a unique set of signs and symptoms, even within families.
Longterm Course
Key Findings
- Skin
Thick, painful calluses on soles, less commonly on palms; variable redness around calluses - Hair
No shaft abnormalities or alopecia - Nails
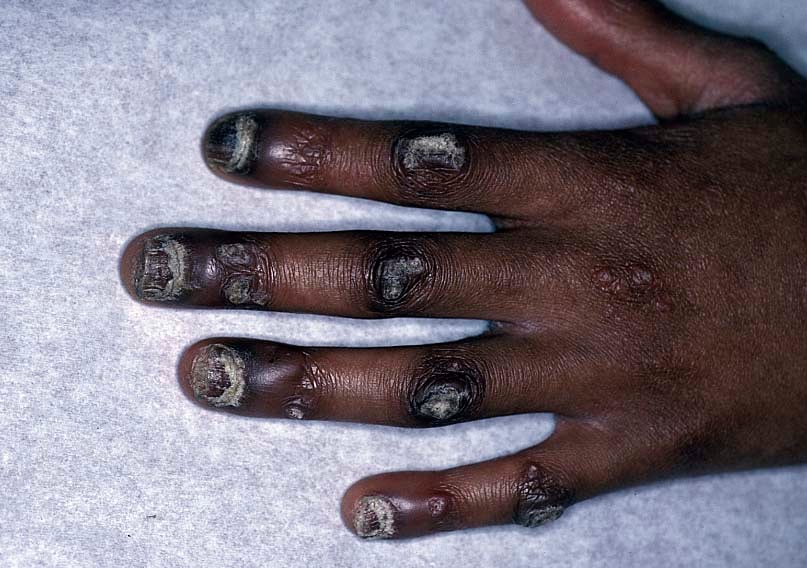
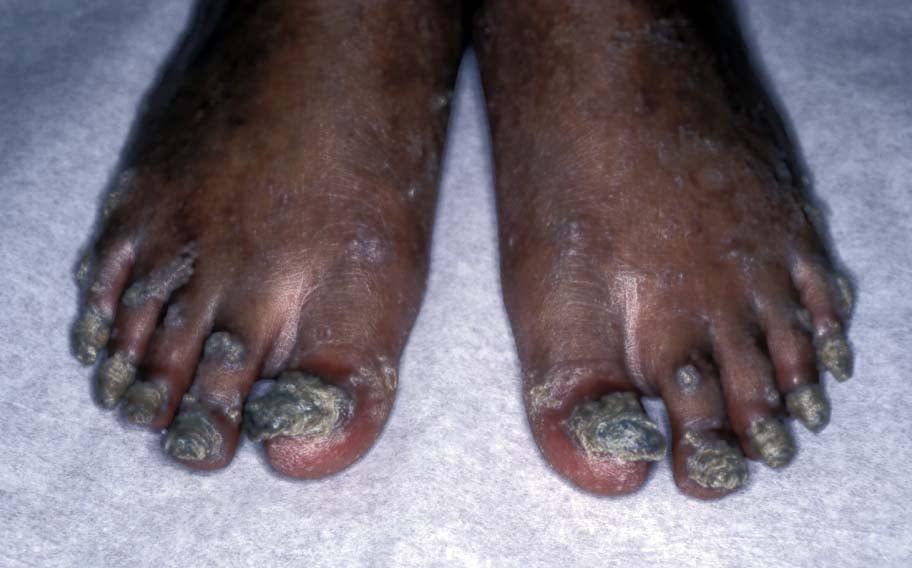
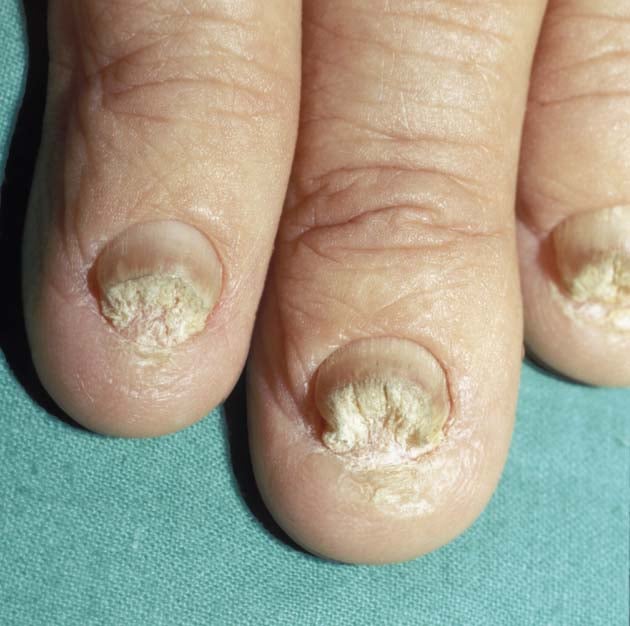
Thickened and hyperconvex
Associated Findings
- Blisters, follicular keratoses, cysts, white patches in mouth, natal teeth
What are the Signs & Symptoms?
- Painful plantar keratoderma – blisters and thick calluses on the soles of the feet causing extreme pain.
- Thickened fingernails and toenails (not necessarily 20/20 nail dystrophy and some have no affected fingernails).
- Cysts – including steatocystoma (epithelial/skin) and other forms of cysts (more likely PC-K17 and PC-K6a). These cysts, when inflamed, can be painful and even debilitating.
- Palmar keratoderma – blisters and thick calluses on the palms of the hands (more likely PC-K16).
- Oral leukokeratosis – thick white plaque on the tongue and the insides of the cheeks (more likely PC-K6a).
- Follicular hyperkeratosis – bumps that form around the hair follicles (more likely PC-K6a).
- Possible involvement of the larynx – hoarseness or thickening of the voice box (more likely PC-K6a).
- Natal or prenatal teeth (associated with PC-K17).
Because of the many similar disorders, often the only way to ensure a patient has PC is for that patient to receive genetic testing. Genetic testing for PC, done through a saliva kit, is currently provided free through the International Pachyonychia Congenita Research Registry at https://www.pachyonychia.org/patient-registry/.
When patients register with the patient advocacy group Pachyonychia Congenita Project (PC Project) through the PC Registry, not only are they able to receive genetic testing, they are invited to be part of the worldwide PC community, which gives them access to patient advocates, help from physicians who are knowledgeable about PC, monthly patient news briefs, a private social media group, and the opportunity to attend patient support meetings. With a disease as rare and isolating as PC, being part of the PC community is often beneficial and even life-changing for some patients and their caregivers.
What is the Treatment?
The most effective factor for PC care is consistent trimming of the nails and the calluses on the feet and sometimes on the palms of the hands. Known as “debridement,” this trimming must not leave the nails too short or too long, and the calluses not too thick and not too thin. When inflamed, cysts may need to be lanced, drained or removed by a physician. As the hyperkeratosis may occur as a reaction to stress or pressure, many patients have found ways to lessen the trauma to feet and hands through special shoes, socks, gloves, insoles or orthotics, crawling, canes, crutches, and other walking aids.
More information and help can be found at www.pachyonychia.org
Clinical Resources
- Clinicians seeking to confirm a diagnosis should visit the Edvyce portal to submit a case to experts in ichthyosis.
- Learn more about FIRST’s Resources for individuals and families affected by Ichthyosis?
- Information about current clinical trials and research studies can be found here.
- Congenital Ichthyosiform Erythroderma (CIE)
- Lamellar Ichthyosis
- Collodion Baby
- Darier Disease
- Epidermal Nevus
- Epidermolytic Ichthyosis
- Erythrokeratodermia Variabilis
- Erythrokeratodermia Cardiomyopathy Syndrome
- Harlequin Ichthyosis
- Ichthyosis Vulgaris
- Ichthyosis with Confetti
- Keratitis-Ichthyosis-Deafness (KID)
- Netherton Syndrome
- Pachyonychia Congenita
- Palmoplantar Keratodermas
- Sjögren-Larsson Syndrome
- X-Linked Ichthyosis
- Chanarin Dorfman Syndrome
- CHILD Syndrome
- Conradi-Hünermann
- Ichthyosis Hystrix with Deafness (HID) Syndrome
- Ichthyosis Hystrix Curth-Macklin
- Refsum Disease
- Trichothiodystrophy
Phenotype Names
Pachyonychia congenita, PC-16 (PC1), PC17 (PC2), PC6a (PC3), PC6b (PC4)
EDD Name
KRT6A-pEDD
KRT6B-pEDD
KRT6C-pEDD
KRT16-pEDD
KRT17-pEDD
OMIM
Inheritance
Autosomal dominant
Incidence
Rare
Diagnostic Tests
Lifelong; may worsen during first 20 years; generally stable thereafter Diagnostic tests: genetic testing is available
Age of First Appearance
none
Abnormal Genes
KRT6A; KRT6B; KRT6C; KRT16; KRT17
Primary Symptom Photos